Teledermatology: Bridging the gap in dermatological care
This article gives you an overview of what teledermatology is, and how you can get started offering online consultations to your patients via Miiskin.
Table of Content
What is teledermatology? | Statistics | Types | Applications | Patient-initiated-teledermatology | The use of AI | Miiskin a teledermatology platform for dermatologists | How to get started with teledermatology | Frequently asked questions
What is Teledermatology?
Teledermatology enables dermatologists to diagnose, monitor, and manage skin conditions remotely using HIPAA-compliant, telehealth platform. Due to its visual nature, dermatology is especially suited for virtual care, allowing high-quality images and patient input to replace in-person visits.
Why is the adoption of teledermatology important for private dermatology clinics?
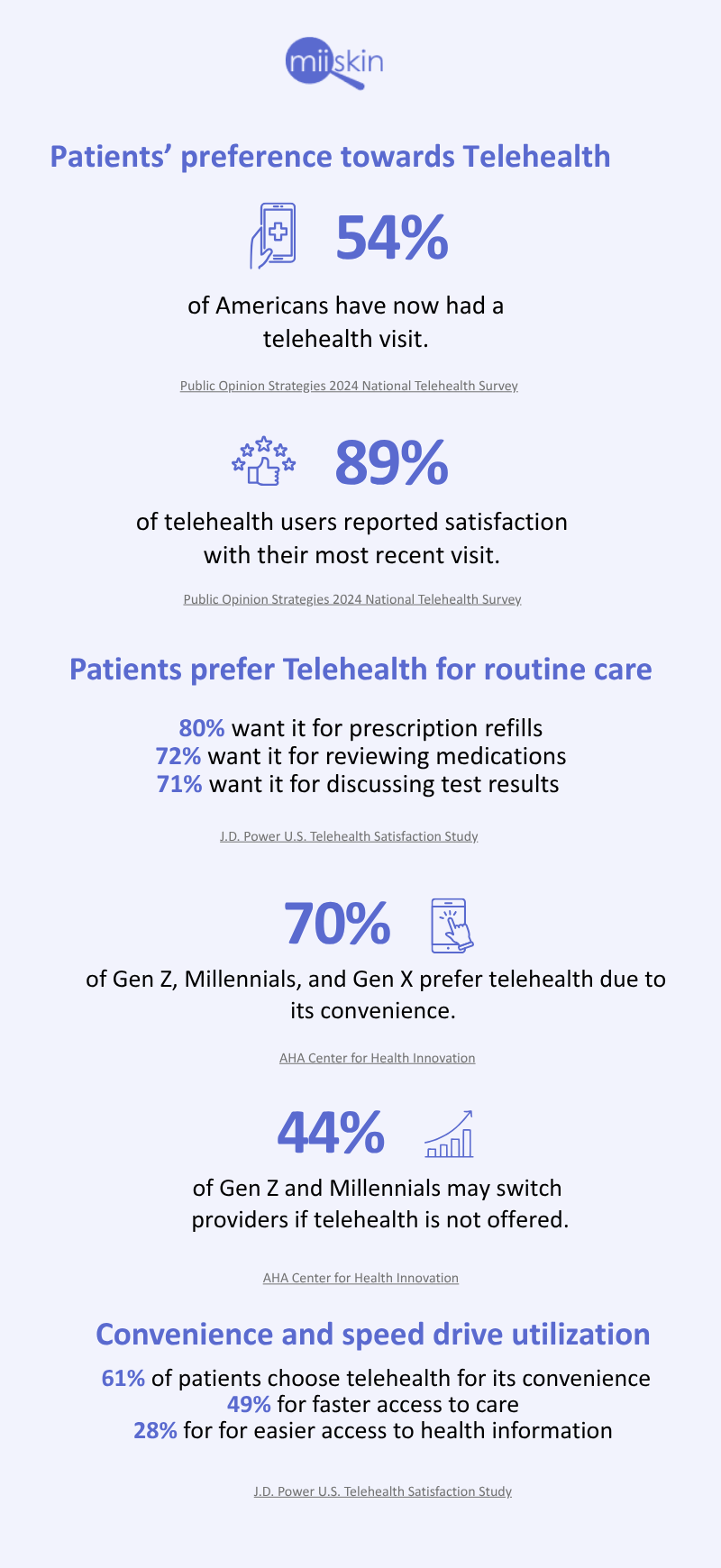
Patients are increasingly frustrated with the long waiting times at traditional dermatology clinics, often facing delays of weeks or even months for appointments. As a result, many are turning to online consultations since they can get faster, more convenient access to care. If private dermatology practices want to remain competitive and avoid losing patients to these online services, they must adapt by integrating teledermatology into their practices. Embracing virtual care not only meets patient expectations for timely service but also helps clinics retain and attract a broader patient base in an increasingly digital healthcare landscape.
What are the types of Teledermatology?
Store-and-forward (Asynchronous) Teledermatology
Store-and-forward teledermatology is the most commonly used modality. It involves capturing high-quality clinical images of a patient’s skin condition, along with relevant medical history, and sending them to a dermatologist for review at a later time. This method does not require the patient and dermatologist to be present simultaneously, making it highly flexible and efficient. It is particularly well-suited for routine consultations, follow-ups, triaging cases, or remote areas where immediate specialist access may be limited.
Real-time (Synchronous) Teledermatology
Real-time teledermatology uses live video conferencing to connect patients and dermatologists for face-to-face consultations in real time. This interactive approach allows dermatologists to ask questions, examine the skin visually, and provide immediate feedback or treatment recommendations. While it requires both parties to be available simultaneously and relies on stable internet connectivity, it can be useful for complex cases, when a dynamic discussion is needed, for example when Accutane is being prescribed for severe acne.
Hybrid Teledermatology
Hybrid teledermatology combines elements of both store-and-forward and real-time methods. Typically, patients first send images and information about their symptoms to the dermatologist, who reviews the material before a scheduled video consultation. This model enables dermatologists to prepare in advance and conduct more informed and focused live consultations. Hybrid approaches offer a balance between convenience and interactivity, making them ideal for comprehensive evaluations that require both image review and direct patient engagement.
Mobile Teledermatology
Mobile teledermatology refers to the use of smartphones and smartphone apps for dermatology to deliver care. Although it can support both asynchronous and synchronous interactions, it is often highlighted separately due to its unique advantages and widespread accessibility. Patients can capture and send images, join video calls, or use mobile apps to connect with dermatologists—often with little more than a cellular data connection. Mobile teledermatology is especially valuable in rural, underserved, or low-resource settings where traditional telemedicine infrastructure may be lacking.
Which type of teledermatology is better for private practices?
For private dermatology practices, asynchronous teledermatology—such as the model offered by platforms like Miiskin—often proves to be the most effective and efficient option. Unlike live video consultations, asynchronous systems allow patients to securely upload images and information about their skin concerns at any time, which dermatologists can then review and respond to at their convenience. This flexibility gives clinicians greater control over their schedules, enabling them to manage cases without the constraints of real-time appointments. For patients, it offers a faster, more accessible way to receive expert care without the hassle of scheduling or travel. By adopting an asynchronous approach, private practices can streamline workflows, enhance patient satisfaction, and maintain a competitive edge in today’s evolving digital healthcare environment.
FOR DERMATOLOGISTS IN USA
Want a steady stream of new patients every month?
Partner with Miiskin and start receiving a steady stream of new patients — simply by joining the platform!
✅ You must have a private practice
✅ You must have your own malpractice insurance (we can help you set-up one)
There’s no upfront subscription — just a $10 usage fee.
Boost your revenue starting today!
Teledermatology applications and functions
Teledermatology is used across a range of healthcare settings and patient populations, and it enables various clinical functions that improve access, efficiency, and continuity of dermatologic care. Understanding both the applications (contexts where teledermatology is used) and the functions (specific tasks it enables) helps clarify its full value in modern healthcare.
1. Clinical diagnosis and management of simple skin diseases
Application:
- Used for evaluating and managing remotely acute or chronic skin diseases such as acne, eczema, psoriasis, among others.
- Supports routine consultations, treatment plans, and disease monitoring.
Functions:
- Virtual consultations
- Online patient triage to determine severity and urgency.
- Virtual prescription renewals based on submitted updates.
- Patient follow-up care for chronic or recurrent conditions.
2. Primary care and specialist referral
Application:
- Primary care providers or nurses capture and send images to dermatologists for expert input.
- Common in general practice or low-resource settings with limited specialist access.
Functions:
- Specialist referral for diagnostic confirmation or management guidance.
- Triage support to prioritize in-person vs. remote management.
- Asynchronous consults for non-urgent dermatologic issues.
3. Rural and underserved area access
Application:
- Expands dermatologic services to geographically isolated or underserved populations.
- Helps overcome barriers like travel distance and shortage of specialists.
Functions:
- Store-and-forward consultations initiated by local clinics or patients.
- Real-time virtual visits when infrastructure allows.
- Education and training for local healthcare workers.
4. Home care and long-term care facilities
Application:
- Used in nursing homes, rehabilitation centers, and home-based care settings.
- Reduces the need to transport patients for routine dermatologic evaluations.
Functions:
- Virtual consultations initiated by caregivers or facility staff.
- Ongoing follow-up care for chronic conditions.
- Prescription renewals and wound or lesion monitoring.
Can you address all these use-cases via the Miiskin platform?
Private dermatology practices can effectively address the full range of teledermatology applications and functions through the Miiskin platform, which is specifically designed to support asynchronous care. With Miiskin, dermatologists can remotely diagnose and manage common skin conditions like acne, eczema, and psoriasis by reviewing patient-submitted images and symptom details, allowing for timely treatment plans, virtual follow-ups, and prescription renewals without the need for real-time consultations.
The platform also facilitates collaboration with primary care providers by enabling efficient triage and specialist referrals, particularly useful in low-resource or general practice settings. For patients in rural or underserved areas, Miiskin’s store-and-forward capabilities eliminate geographic barriers, making expert dermatologic care accessible without requiring travel.
Additionally, the platform supports long-term care and home-based settings, where caregivers or facility staff can initiate consultations, monitor chronic conditions, and renew treatments seamlessly. By adopting Miiskin, private practices can streamline workflows, expand access, and deliver high-quality, patient-centered dermatologic care across diverse scenarios.
FOR DERMATOLOGISTS IN USA
Want a steady stream of new patients every month?
Partner with Miiskin and start receiving a steady stream of new patients — simply by joining the platform!
✅ You must have a private practice
✅ You must have your own malpractice insurance (we can help you set-up one)
There’s no upfront subscription — just a $10 usage fee.
Boost your revenue starting today!
What is patient-initiated Teledermatology?
Patient-initiated teledermatology is a model of dermatologic care in which the patient initiates a remote consultation with a dermatologist—without needing a referral. It’s often delivered through mobile apps, online platforms, or healthcare portals, and allows patients to submit photos and information about their skin concerns on their own schedule.
How does patient-initiated Teledermatology work?
- The patient identifies a skin concern.
- They upload photos and a brief description of symptoms through a teledermatology platform, such as Miiskin.
- A dermatologist reviews the case—often asynchronously—and provides a diagnosis, treatment plan, or prescription.
- Follow-up care or messaging is also included in the Miiskin platform.
Key features of patient-initiated Teledermatology
- Direct access to dermatologists without going through a primary care provider.
- Typically asynchronous (store-and-forward), but may include live video consultations if needed.
- Allows for quick feedback, sometimes within a day.
- Increasingly used for chronic skin condition follow-ups, prescription renewals, and urgent but non-life threating skin issues.
Why patient-initiated Teledermatology is growing
- Smartphones and digital cameras make it easy for patients to take high-quality images.
- Post-COVID-19 telehealth expansion increased comfort with virtual care.
- Meets demand for convenient, on-demand dermatology, especially among younger, tech-savvy patients.
Considerations
- Image quality is critical—patients must be guided on how to take clear photos.
- Not all skin conditions can be safely diagnosed without an in-person exam.
Use cases of patient-initiated Teledermatology
- Diagnostic and treatment of routine skin conditions such as acne, rosacea, eczema, etc.
- Prescription refills for ongoing dermatologic treatments.
- Cosmetic consultations for example, anti-aging, hair loss or hyperpigmentation.
- Suspicious moles or new skin lesions
The use of AI in teledermatology
The use of AI in teledermatology is gaining momentum, particularly in streamlining clinical workflows and improving patient care. A notable example is Miiskin, a telehealth company that recently earned an Innobooster grant to advance its AI-driven dermatology platform.
The Miiskin system will leverage deep learning and large language models to assess acne severity, skin type, and treatment needs in under 60 seconds—with diagnostic accuracy around 90%.
The AI not only identifies the skin condition but also proposes personalized treatment plans and follow-up recommendations, all of which can be reviewed and approved by a dermatologist in a single click.
By automating routine tasks—such as analyzing images, generating diagnoses, and drafting management suggestions—AI eases provider workloads, supports faster patient access, and enhances consistency in care delivery.
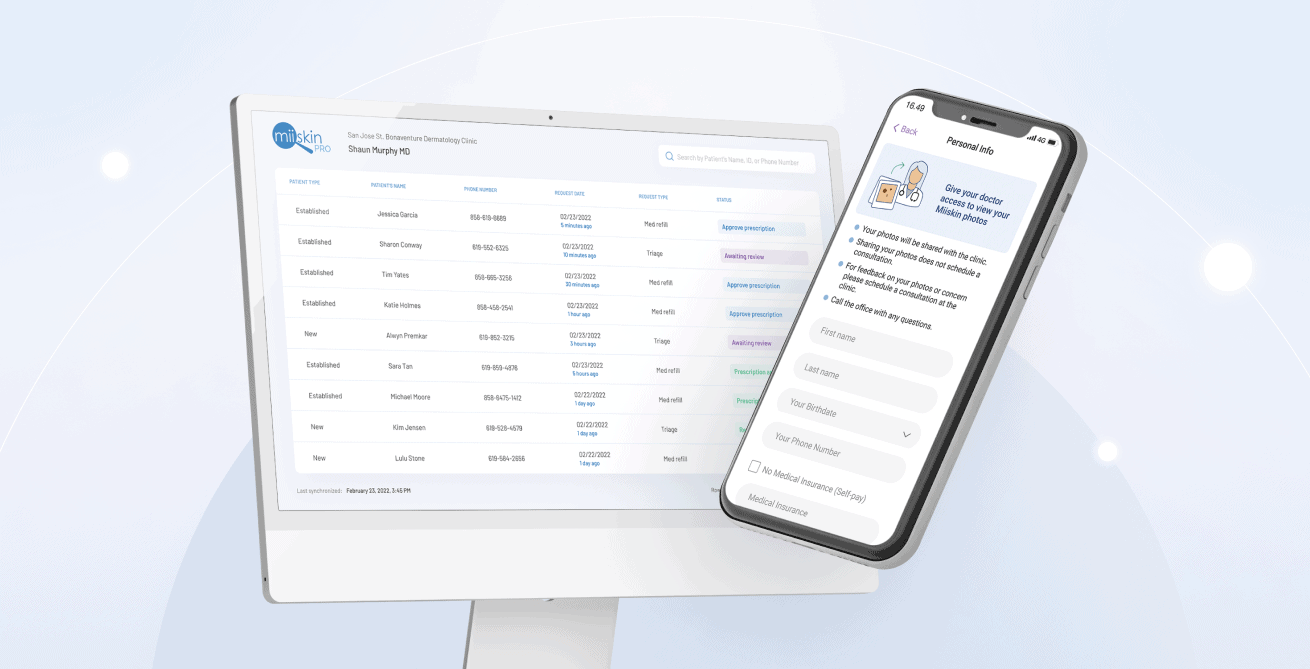
Miiskin a Teledermatology platform for private dermatology practices
The Miiskin platform is ideal for private dermatology practices for several compelling reasons:
- On-demand access anytime, anywhere: Patients can easily take and upload images of their skin concerns—no appointment necessary. This direct, consumer-led model empowers patients to seek expert evaluation exactly when they need it.
- Asynchronous, easy-to-use workflow: Miiskin’s store‑and‑forward system lets dermatologists review cases at their convenience—between in‑office visits or from anywhere—offering unmatched flexibility and efficiency for busy private practices.
- Prescription capability: Via the Miiskin platform dermatologists can send electronic prescriptions to the pharmacy of the patient’s choice.
- Built for clinical and operational effectiveness: The platform supports virtual triage, diagnosis, follow-up, and e-prescriptions. It returns most consultations within 24–48 hours, helping with acute concerns and routine management of chronic conditions .
- Secure, HIPAA-compliant, and trusted: Fully HIPAA-compliant and LegitScript-certified, Miiskin ensures patient data is protected. Its accreditation by the Skin Health Alliance and use by over 130 clinics globally speak to its professional reliability.
- Enhances patient engagement and clinic growth: Patients stay connected— with follow-up appointments—creating deeper clinical relationships. Many providers have expanding their patient base by engaging this digital audience.
How to get started with the Miiskin platform?
In order to get started you need to have your own private practice, licenses in at least 3 states and your own malpractice insurance. If you meet these 3 requirements, getting started with the Miiskin platform is very easy, just set-up a call and in just a few days you can start receiving your first teledermatology consultation. Read about three dermatologists who have successfully started thriving online practices with Miiskin.
FOR DERMATOLOGISTS IN USA
Want a steady stream of new patients every month?
Partner with Miiskin and start receiving a steady stream of new patients — simply by joining the platform!
✅ You must have a private practice
✅ You must have your own malpractice insurance (we can help you set-up one)
There’s no upfront subscription — just a $10 usage fee.
Boost your revenue starting today!
Frequently asked questions about teledermatology
How effective is teledermatology?
When Teledermatology is conducted by board-certified dermatologists, (like in the case of Miiskin) who have extensive experience in virtual care it is highly effective, particularly for diagnosing and managing common skin conditions. Numerous studies have shown that its diagnostic accuracy is comparable to in-person consultations, especially when high-quality images are provided 1. It improves access to specialist care, reduces wait times, and facilitates timely interventions, especially in remote or underserved areas. While not a replacement for all face-to-face visits, teledermatology is a reliable and efficient tool for many dermatologic needs.
What is the process of teledermatology?
The teledermatology process typically begins with the patient or a referring provider capturing and submitting clinical images of the skin concern along with relevant medical history. These are then reviewed by a dermatologist either asynchronously (store-and-forward) or during a live video consultation (synchronous). After evaluation, the dermatologist provides a diagnosis, treatment plan, or recommendation for further follow-up. Patients receive results and care instructions through the HIPAA-compliant Miiskin platform and patients can write questions and concerns to the dermatologist directly through the platform.
How long do teledermatology results take?
The turnaround time for teledermatology results depends on the dermatologist, but via the Miiskin platform, doctors provide feedback within 24 to 48 hours. For example, Miiskin reports that 90% of online consultations are reviewed by a dermatologist in less than 24 hours, although results may take up to two business days during high-volume periods or holidays.
What happens after teledermatology?
After a teledermatology consultation via Miiskin, the patient typically receives a diagnosis or clinical opinion, along with a treatment plan. This may include starting or adjusting medications, receiving prescriptions, or monitoring the condition at home. If the case is complex or unclear, the dermatologist may recommend an in-person follow-up for further examination, or lab tests. The Miiskin platforms also provides follow-up messaging to ensure treatment effectiveness and address new symptoms.
What is the use of teledermatology?
Teledermatology is used to diagnose, monitor, and manage skin conditions remotely, offering a convenient alternative to in-person visits, often at a more affordable price. It improves access to dermatologic care for patients in rural or underserved areas, facilitates faster triage and referrals, supports chronic condition follow-ups, and allows for efficient prescription management. It’s also valuable in home care settings, long-term care facilities, and hospitals lacking full-time dermatologists.
What are the modalities of teledermatology?
Teledermatology is delivered through three main modalities: store-and-forward (asynchronous), where images and information are submitted and reviewed later; real-time (synchronous), which involves live video consultations; and hybrid models, which combine both approaches. These modalities can be accessed via desktop platforms, mobile apps, or integrated healthcare systems, depending on patient preference and clinical context.
Does insurance cover telemedicine?
Most direct-to-consumer telemedicine platforms, including Miiskin, do not accept insurance. However, their prices are often lower than the out-of-pocket cost of an in-person visit—sometimes even less than a typical specialist co-pay. For example, with Miiskin, you can consult a board-certified dermatologist for just $39 to $59 per visit, without subscriptions or hidden fees. That’s convenient, affordable care—no insurance required.
How much is the average dermatologist visit without insurance?
The average cost of a dermatologist visit without insurance in the U.S. typically ranges from $100 to $250, depending on factors like location, provider fees, and the nature of the visit. For patients paying out-of-pocket, this can be a significant expense. As a more affordable alternative, platforms like Miiskin offer access to board-certified dermatologists for just $39 to $59 per consultation, with no subscriptions or insurance required—making expert skin care more accessible and budget-friendly.
Do doctors like telemedicine?
Yes, many doctors—especially dermatologists—appreciate the flexibility and efficiency that telemedicine offers, particularly through asynchronous platforms like Miiskin. Unlike traditional appointments, asynchronous care allows providers to review cases on their own schedule, whether between appointments, after hours, or from home. With detailed patient questionnaires and high-quality images submitted through the platform, dermatologists have all the information they need to deliver accurate, personalized care—without the pressure of live consultations. This model not only improves work-life balance but also helps doctors serve more patients without sacrificing clinical quality.
Are you a dermatologist who wants to learn more about teledermatology?
Check out our articles on Teledermatology
Teledermatology: Bridging the gap in dermatological care
Embracing Teledermatology: What three dermatologists learned firsthand
How store and forward telehealth supports direct-to-consumer healthcare
7 Teledermatology apps doctors should know about
5 Teledermatology companies to choose from based on your needs
Choosing the right teledermatology software



 Join the Miiskin network and get new patients every month!
Join the Miiskin network and get new patients every month!
